- Book A No-Cost Consultation
- What Is Medicaid?
- Are Braces Covered By Wisconsin Medicaid?
- How To Qualify For Medicaid Wisconsin Braces?
- Eligibility Criteria
- How To Go About Medicaid Braces Treatment In Wisconsin
- What Are Other Plans Available For Wisconsin Braces?
- What Is A BadgerCare Plus Dental Program?
- BadgerCare Eligibility Requirements
- Wisconsin Medicaid And BadgerCare Plus Non-Emergency Medical Transportation
- Braces Covered By Trilogy Health Insurance In Wisconsin
- If You Already Have A Dentist
- Insurances That We Accept
Medicaid orthodontic program provides comprehensive dental coverage for their patients. Dental treatments may include treatment for pain and infections, teeth restoration treatments, and regular check-ups and cleanings. For orthodontics, however, very few patients requiring braces, or any other dental service will qualify for coverage unless their condition is deemed medically necessary.
Orthodontic Experts believe that everyone should have a right to smile perfectly and shouldn’t miss any opportunity of having a beautiful smile therefore we have got interest-free financing options with low monthly payments to make this dental treatment affordable for you. We also have many options for braces to meet your individual needs.

Book a No-Cost consultation
What is Medicaid?
Medicaid is basically a state-run and federally funded program that offers affordable health coverage to eligible adults, children, pregnant women, elderly adults, and people with disabilities. It’s an assistance program designed for healthcare to low-income families and individuals who may not be able to afford expensive healthcare treatments.

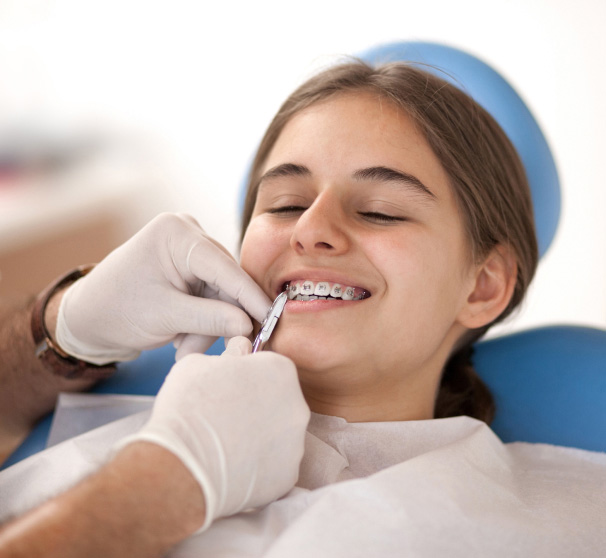
Are Braces covered by Wisconsin Medicaid?
The Medicaid approval process for dental care depends on various factors such as the age of the patient, current oral health condition, and the type of orthodontic treatment required. Medicaid covers dental care and orthodontic services, like braces, when they are deemed medically necessary for your child. Some examples include cases that consist of a cleft palate or severe anomalies of the face that can’t be adjusted without braces.
The first steps in finding out if you are qualified would be getting a referral from your primary dentist for an examination with an orthodontist, though it is not necessary and we would be more than happy to see you if you do not have a referral. The administrators of the State of Wisonsin Medicaid are required to pre-approve all children for braces coverage before orthodontic treatment can begin.
Additional pre-orthodontic services that can be covered include extractions and restorations, and these services would be provided by a dentist. We believe everyone should have the opportunity for a Dream Smile, so we are always available to help you navigate your coverage.
However, just because a patient may have moderate or severe orthodontic issues, and/or has been advised by a dental professional that they need braces, this does not mean that the patient will qualify for coverage.
How to qualify for Medicaid Wisconsin braces?
Braces would be necessitated only if without the treatment, the condition would become more severe and result in pain, infection, illness, or significant and immediate impact on the normal function of the body and the patient’s inability to function normally.
Orthodontic Treatment Not Deemed Medically Necessary Are
- Braces required only for aesthetic reasons
- Treatment required to correct crowded teeth
- The patient has demonstrated a lack of motivation to maintain standards of oral hygiene and oral hygiene is deficient
Orthodontic braces can often cost up to $8,000 and since only a few families can afford to pay an $8,000 dental bill, you should look for ways to qualify for free or discounted braces. Even if you can’t find free options in your area, you can always make braces more affordable by getting a discounted dental plan.
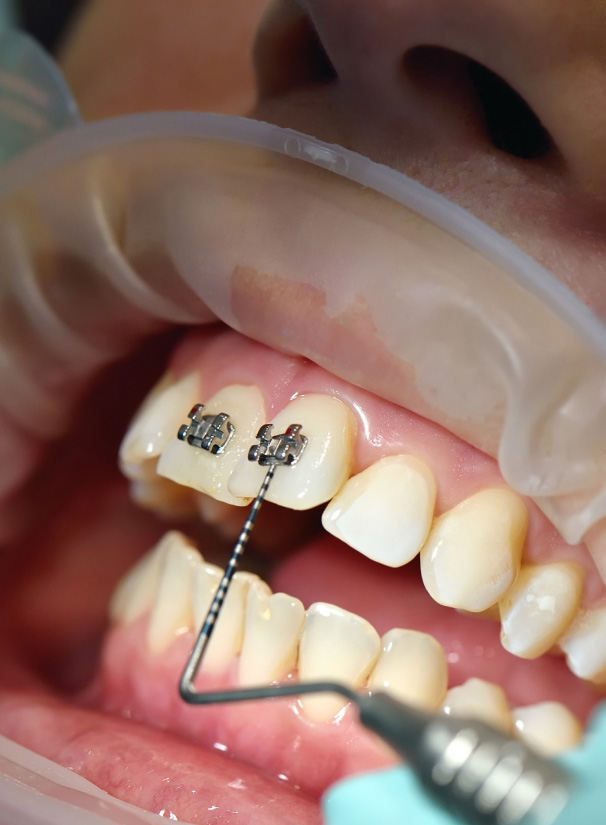
If you qualify for Medicaid or the (CHIP) Children’s Health Insurance Program, then your Wisconsin state government may pay for you or your children to get braces. If your family doesn’t qualify for free braces through Medicaid or CHIP, then you should consider getting a dental plan that will lower orthodontic prices. Dental plans can help you save a considerable amount of money on braces for children and adults. Once you have a Dental plan, you get a discounted rate for all of your dental needs, including orthodontics.
Eligibility Criteria
It is important to understand that Medicaid will only cover orthodontic braces for children under 21. Although, there are now some dental benefits for adults with Medicaid, but this does not extend to braces or orthodontics. So, if you are an adult with Medicaid and want braces, we can definitely assist you, but realize that your Medicaid insurance will not help with the costs.
However, Medicaid will pay for the costs of braces in full for children under 21, if they determine that the need for medically necessary braces exists. You can have your child be evaluated for this medical necessity once per year. If they get reviewed for braces and are denied, you can try again– but you must wait one year in between evaluations. Typically, they will allow three attempts. If they are denied before they have all their adult teeth, it may be a good idea, depending on your finances, to wait a year and try again. If they are denied after they have all their teeth, we typically cannot apply again, and it would likely be time to discuss private financing. (We offer a discount to these cases along with interest-free financing).
All orthodontic services require Prior authorization (PA) by the Wisconsin Medicaid. This PA will decide the reimbursement to the approved service.

Imagine the Possibilities, Even When Denied. Braces for Just $195/Month with No Down Payment
*Terms and Conditions apply. Must have state denial status or letter. An initial payment of $195 Is due on the day of placing braces, the rest of the payments will be completed via recurring monthly payments until the minimum amount has been remitted. Automatic deductions for the monthly payments must be set up. Metal braces only. Not applicable to patients with an active payment plan.
How to go about Medicaid braces treatment in Wisconsin
You may need to schedule a no-cost initial assessment appointment with our staff and make sure that you inform us about your Medicaid Coverage. It will be critical to know that you are still covered on the day of this initial assessment.
- At this first assessment, we will take the photos and X-rays needed by Medicaid for them to make an evaluation along with filling out a report for them detailing our findings.
- These reports will be sent to the Medicaid for evaluation of the case and typically they will provide their determination within four to six weeks.
- They will notify both our office and your family by mail. If they deny, and we noted in our report that the case was extremely severe, we may choose to appeal. If the appeal is denied, your family has the further right to appeal.
- If approved, you would call our offices and make an appointment. As long as you have Medicaid coverage on the day of the appointment, Medicaid will then cover the cost of treatment in full.

So when should you bring your kids? The American Association of Orthodontics says see your orthodontist for your first visit by age 7 because there is a lot we can do at that early age.
What are other plans available for Wisconsin Braces?
Orthodontic Experts perform orthodontic treatments if you have any of these plans available in Wisconsin Medicaid, iCare, Trilogy, and BadgerCare Plus.

What is a BadgerCare Plus dental program?
BadgerCare Plus is a similar program for groups of people who may not qualify for Medicaid or have different needs for healthcare coverage. BadgerCare Plus is also sometimes informally referred to as just BadgerCare. BadgerCare plus is a healthcare program for all low-income and disable residents of Wisconsin who are elderly, blind or disabled but still need healthcare coverage. It does not have an open enrollment period, and people can apply at any time.
BadgerCare Eligibility
Requirements
Wisconsin BadgerCare plus dental services are only available to the children under the age of 18 years and pregnant women as well as adult ages between 18-25 years who were in foster care. BadgerCare plus reimbursement is allowed only for services that meet all program requirements. Orthodontia diagnosis only is however allowed for the members ages 21 and over. Groups that are eligible for BadgerCare plus are:
- All children under age 19, regardless of income.
- Pregnant women with incomes up to 300% of the Federal Poverty Level (FPL).
- Parents and relatives caring for a child up to 200% of the FPL.
- Young adults in foster care who turn 18 on or after January 1, 2008, will automatically be able to get BadgerCare until they turn 21, regardless of income.
- Farm families and other families who are self-employed may be eligible under BadgerCare if their income is under 200% of the FPL.
- Parents whose child/children are in foster care and who have a reunification plan in place may be eligible for BadgerCare if their income is below 200% of the federal poverty level.
Wisconsin Medicaid and BadgerCare Plus Non-Emergency Medical Transportation
Who can call Non-Emergency Medical Transportation?
Non-emergency medical transportation is a public transportation, which provides a shared ride in either specialized medical services or other types depending on your medical and transportation needs.
If you are enrolled into any of these programs, you may be able to book a ride with Medical Transportation Management (MTM), Inc, who schedules and pays for your rides as your Medicaid and BadgerCare Plus transportation manager, in case you do not get a free ride.
- Wisconsin Medicaid including IRIS
- BadgerCare Plus
- Family Planning
- Tuberclosis related services
- Express enrollment for BadgerCare plus r family planning only services

Similarly, if you are able to drive to your appointment but cannot afford to pay for gas, you may contact MTM, Inc, to check if you can be reimbursed for mileage.
For further information on scheduling rides, meals and lodging, complaints, new rules and denied transportation contact MTM on following numbers:
- 1-866-907-1493 (Voice) or 711 (TTY)
- Call member services at 1-800-362-3002
To know more visit: https://www.mtm-inc.net/Wisconsin/
Braces covered by Trilogy health insurance in Wisconsin
Trilogy is a healthcare insurance plan that is responsible for providing all medically necessary services under BadgerCare plus and Medicaid SSI. For Trilogy members in Wisconsin dental services are a covered benefit under BadgerCare Plus so typically you will get the braces covered. You may get covered dental services from a Medicaid-enrolled provider who will accept your Forward Health ID card. You may be charged a copayment for these services.
If you have a dental emergency, you have the right to obtain treatment within 24 hours of your request with any trilogy health insurance providers.
A dental emergency is a need for immediate dental services to treat severe dental pain, swelling, fever, infection, or injury to the teeth.
If you are experiencing a dental emergency:
If you already have a dentist:
- Call the dentist’s office.
- Tell the dentist’s office that you or your child is having a dental emergency.
- Tell the dentist’s office what the exact dental problem is. This may be something like a severe toothache or swollen face.
If you do not currently have a dentist:
- Call ForwardHealth Member Services at 1-800-362-3002.
- Tell them that you/your child is having a dental emergency. They can help you get dental services.
- You can see any dentist who will accept your ForwardHealth card.
Trilogy insurance services ensure that the dental patient gets the treatment on time and within the dental insurance health plans.








